Schizophrenia (2 of 3):
Schizophrenia (/ˌskɪtsɵˈfrɛniə/ or/ˌskɪtsɵˈfriːniə/) is a mental disorder often characterized by abnormal social behavior and failure to recognize what is real. Common symptoms include false beliefs, unclear or confused thinking, auditory hallucinations, reduced social engagement and emotional expression, and lack of motivation. Diagnosis is based on observed behavior and the person's reported experiences..
Causes
Main article: Causes of schizophrenia
A combination of genetic and environmental factors play a role in the development of schizophrenia.[1][4] People with a family history of schizophrenia who have a transient psychosis have a 20–40% chance of being diagnosed one year later.[28]
Genetic
Estimates of heritability vary because of the difficulty in separating the effects of genetics and the environment;[29] averages of 0.80 have been given.[30] The greatest risk for developing schizophrenia is having a first-degree relative with the disease (risk is 6.5%); more than 40% of monozygotic twins of those with schizophrenia are also affected.[1] If one parent is affected the risk is about 13% and if both are affected the risk is nearly 50%.[30]
It is likely that many genes are involved, each of small effect and unknown transmission and expression.[1] Many possible candidates have been proposed, including specific copy number variations, NOTCH4, and histone protein loci.[31] A number of genome-wide associations such as zinc finger protein 804Ahave also been linked.[32] There appears to be overlap in the genetics of schizophrenia andbipolar disorder.[33] Evidence is emerging that the genetic architecture of schizophrenia involved both common and rare risk variation.[34]
Assuming a hereditary basis, one question from evolutionary psychology is why genes that increase the likelihood of psychosis evolved, assuming the condition would have been maladaptive from an evolutionary point of view. One idea is that genes are involved in the evolution of language and human nature, but to date such ideas remain little more than hypothetical in nature.[35][36]
Environment
Environmental factors associated with the development of schizophrenia include the living environment, drug use and prenatal stressors.[4] Parenting style seems to have no major effect, although people with supportive parents do better than those with critical or hostile parents.[1] Childhood trauma, death of a parent, and being bullied or abused increase the risk of psychosis.[37] Living in an urban environment during childhood or as an adult has consistently been found to increase the risk of schizophrenia by a factor of two,[1][4]even after taking into account drug use,ethnic group, and size of social group.[38]Other factors that play an important role include social isolation and immigration related to social adversity, racial discrimination, family dysfunction, unemployment, and poor housing conditions.[1][39]
Substance use
About half of those with schizophrenia use drugs or alcohol excessively.[40]Amphetamine, cocaine, and to a lesser extent alcohol, can result in psychosis that presents very similarly to schizophrenia.[1][41] Although it is not generally believed to be a cause of the illness, people with schizophrenia usenicotine at much greater rates than the general population.[42]
Alcohol abuse can occasionally cause the development of a chronic substance-induced psychotic disorder via a kindling mechanism.[43] Alcohol use is not associated with an earlier onset of psychosis.[44]
A significant proportion of people with schizophrenia use cannabis to help cope with its symptoms.[40] Cannabis can be a contributory factor in schizophrenia,[45][46][47]but cannot cause it alone;[47] its use is neither necessary nor sufficient for development of any form of psychosis.[47] Early exposure of the developing brain to cannabis increases the risk of schizophrenia,[45] although the size of the increased risk is difficult to quantify;[45][46] only a small proportion of early cannabis recreational users go on to develop any schizoaffective disorder in adult life,[46]and the increased risk may require the presence of certain genes within an individual[47] or may be related to preexisting psychopathology.[45] Higher dosage and greater frequency of use are indicators of increased risk of chronic psychoses.[46]Tetrahydrocannabinol (THC) and cannabidiol(CBD) produce opposing effects; CBD has antipsychotic and neuroprotective properties and counteracts negative effects of THC.[46]
Other drugs may be used only as coping mechanisms by individuals who have schizophrenia to deal with depression, anxiety, boredom, and loneliness.[40][48]
Developmental factors
Factors such as hypoxia and infection, or stress and malnutrition in the mother duringfetal development, may result in a slight increase in the risk of schizophrenia later in life.[4] People diagnosed with schizophrenia are more likely to have been born in winter or spring (at least in the northern hemisphere), which may be a result of increased rates of viral exposures in utero.[1] The increased risk is about 5 to 8%.[49] Other infections during pregnancy or around the time of birth that may increase the risk include Toxoplasma gondi and Chlamydia.[50]
Mechanisms
Main article: Mechanisms of schizophrenia
A number of attempts have been made to explain the link between altered brain function and schizophrenia.[4] One of the most common is the dopamine hypothesis, which attributes psychosis to the mind's faulty interpretation of the misfiring ofdopaminergic neurons.[4]
Psychological
Many psychological mechanisms have been implicated in the development and maintenance of schizophrenia. Cognitive biases have been identified in those with the diagnosis or those at risk, especially when under stress or in confusing situations.[51]Some cognitive features may reflect globalneurocognitive deficits such as memory loss, while others may be related to particular issues and experiences.[52][53]
Despite a demonstrated appearance of blunted affect, recent findings indicate that many individuals diagnosed with schizophrenia are emotionally responsive, particularly to stressful or negative stimuli, and that such sensitivity may cause vulnerability to symptoms or to the disorder.[54][55] Some evidence suggests that the content of delusional beliefs and psychotic experiences can reflect emotional causes of the disorder, and that how a person interprets such experiences can influence symptomatology.[56][57][58] The use of "safety behaviors" (acts such as gestures or the use of words in specific contexts) to avoid or neutralize imagined threats may actually contribute to the chronicity of delusions.[59]Further evidence for the role of psychological mechanisms comes from the effects ofpsychotherapies on symptoms of schizophrenia.[60]
Neurological
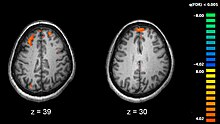
Functional magnetic resonance imaging (fMRI) showing two levels of the brain; areas in orange were more active in healthy controls than in medicated people with schizophrenia.
Schizophrenia is associated with subtle differences in brain structures, found in 40 to 50% of cases, and in brain chemistry during acute psychotic states.[4] Studies usingneuropsychological tests and brain imagingtechnologies such as fMRI and PET to examine functional differences in brain activity have shown that differences seem to most commonly occur in the frontal lobes,hippocampus and temporal lobes.[61]Reductions in brain volume, smaller than those found in Alzheimer's disease, have been reported in areas of the frontal cortex and temporal lobes. It is uncertain whether these volumetric changes are progressive or preexist prior to the onset of the disease.[27]These differences have been linked to theneurocognitive deficits often associated with schizophrenia.[62] Because neural circuits are altered, it has alternatively been suggested that schizophrenia should be thought of as a collection of neurodevelopmental disorders.[63] There has been debate on whether treatment with antipsychotics can itself cause reduction of brain volume.[64]
Particular attention has been paid to the function of dopamine in the mesolimbic pathway of the brain. This focus largely resulted from the accidental finding thatphenothiazine drugs, which block dopamine function, could reduce psychotic symptoms. It is also supported by the fact that amphetamines, which trigger the release of dopamine, may exacerbate the psychotic symptoms in schizophrenia.[65] The influential dopamine hypothesis of schizophrenia proposed that excessive activation of D2receptors was the cause of (the positive symptoms of) schizophrenia. Although postulated for about 20 years based on the D2blockade effect common to all antipsychotics, it was not until the mid-1990s that PET and SPET imaging studies provided supporting evidence. The dopamine hypothesis is now thought to be simplistic, partly because newer antipsychotic medication (atypical antipsychoticmedication) can be just as effective as older medication (typical antipsychoticmedication), but also affects serotoninfunction and may have slightly less of a dopamine blocking effect.[66]
Interest has also focused on the neurotransmitter glutamate and the reduced function of the NMDA glutamate receptor in schizophrenia, largely because of the abnormally low levels of glutamate receptorsfound in the postmortem brains of those diagnosed with schizophrenia,[67] and the discovery that glutamate-blocking drugs such as phencyclidine and ketamine can mimic the symptoms and cognitive problems associated with the condition.[68] Reduced glutamate function is linked to poor performance on tests requiring frontal lobe and hippocampal function, and glutamate can affect dopamine function, both of which have been implicated in schizophrenia, have suggested an important mediating (and possibly causal) role of glutamate pathways in the condition.[69] But positive symptoms fail to respond to glutamatergic medication.[70]
Diagnosis
Main article: Diagnosis of schizophrenia

John Nash, an Americanmathematician and joint winner of the 1994 Nobel Prize for Economics, who had schizophrenia. His life was the subject of the 2001Academy Award-winning filmA Beautiful Mind.
Schizophrenia is diagnosed based on criteria in either the American Psychiatric Association's fifth edition of the Diagnostic and Statistical Manual of Mental Disorders(DSM 5), or the World Health Organization'sInternational Statistical Classification of Diseases and Related Health Problems (ICD-10). These criteria use the self-reported experiences of the person and reported abnormalities in behavior, followed by a clinical assessment by a mental health professional. Symptoms associated with schizophrenia occur along a continuum in the population and must reach a certain severity before a diagnosis is made.[1] As of 2013 there is no objective test.[71]
Criteria
In 2013, the American Psychiatric Association released the fifth edition of the DSM (DSM-5). To be diagnosed with schizophrenia, two diagnostic criteria have to be met over much of the time of a period of at least one month, with a significant impact on social or occupational functioning for at least six months. The person had to be suffering from delusions, hallucinations or disorganized speech. A second symptom could be negative symptoms or severely disorganized or catatonic behaviour.[72] The definition of schizophrenia remained essentially the same as that specified by the 2000 version of DSM (DSM-IV-TR), but DSM-5 makes a number of changes.
- Subtype classifications – such as catatonic and paranoid schizophrenia – are removed. These were retained in previous revisions largely for reasons of tradition, but had subsequently proved to be of little worth.[73]
- Catatonia is no longer so strongly associated with schizophrenia.[74]
- In describing a person's schizophrenia, it is recommended that a better distinction be made between the current state of the condition and its historical progress, to achieve a clearer overall characterization.[73]
- Special treatment of Schneider's first-rank symptoms is no longer recommended.[73]
- Schizoaffective disorder is better defined to demarcate it more cleanly from schizophrenia.[73]
- An assessment covering eight domains ofpsychopathology – such as whether hallucination or mania is experienced – is recommended to help clinical decision-making.[75]
The ICD-10 criteria are typically used in European countries, while the DSM criteria are used in the United States and to varying degrees around the world, and are prevailing in research studies. The ICD-10 criteria put more emphasis on Schneiderian first-rank symptoms. In practice, agreement between the two systems is high.[76]
If signs of disturbance are present for more than a month but less than six months, the diagnosis of schizophreniform disorder is applied. Psychotic symptoms lasting less than a month may be diagnosed as brief psychotic disorder, and various conditions may be classed as psychotic disorder not otherwise specified, while schizoaffective disorder is diagnosed if symptoms of mood disorder are substantially present alongside psychotic symptoms. If the psychotic symptoms are the direct physiological result of a general medical condition or a substance, then the diagnosis is one of a psychosis secondary to that condition.[72]Schizophrenia is not diagnosed if symptoms of pervasive developmental disorder are present unless prominent delusions or hallucinations are also present.[72]
Subtypes
The DSM-5 work group proposed dropping the five sub-classifications of schizophrenia included in DSM-IV-TR:[77][78]
- Paranoid type: Delusions or auditory hallucinations are present, but thought disorder, disorganized behavior, or affective flattening are not. Delusions are persecutory and/or grandiose, but in addition to these, other themes such as jealousy, religiosity, orsomatization may also be present. (DSM code 295.3/ICD code F20.0)
- Disorganized type: Named hebephrenic schizophrenia in the ICD. Where thought disorder and flat affect are present together. (DSM code 295.1/ICD code F20.1)
- Catatonic type: The subject may be almost immobile or exhibit agitated, purposeless movement. Symptoms can include catatonic stupor and waxy flexibility. (DSM code 295.2/ICD code F20.2)
- Undifferentiated type: Psychotic symptoms are present but the criteria for paranoid, disorganized, or catatonic types have not been met. (DSM code 295.9/ICD code F20.3)
- Residual type: Where positive symptoms are present at a low intensity only. (DSM code 295.6/ICD code F20.5)
The ICD-10 defines two additional subtypes:[78]
- Post-schizophrenic depression: A depressive episode arising in the aftermath of a schizophrenic illness where some low-level schizophrenic symptoms may still be present. (ICD code F20.4)
- Simple schizophrenia: Insidious and progressive development of prominent negative symptoms with no history of psychotic episodes. (ICD code F20.6)
Sluggish schizophrenia is in the Russian version of the ICD-10. "Sluggish schizophrenia" is in the category of "schizotypal" disorder in section F21 of chapter V.[79]
Differential diagnosis
Psychotic symptoms may be present in several other mental disorders, includingbipolar disorder,[80] borderline personality disorder,[81] drug intoxication and drug-induced psychosis. Delusions ("non-bizarre") are also present in delusional disorder, and social withdrawal in social anxiety disorder,avoidant personality disorder and schizotypal personality disorder. Schizotypal personality disorder has symptoms that are similar but less severe than those of schizophrenia.[71]Schizophrenia occurs along with obsessive-compulsive disorder (OCD) considerably more often than could be explained by chance, although it can be difficult to distinguish obsessions that occur in OCD from the delusions of schizophrenia.[82] A few people withdrawing from benzodiazepines experience a severe withdrawal syndrome which may last a long time. It can resemble schizophrenia and be misdiagnosed as such.[83]
A more general medical and neurological examination may be needed to rule out medical illnesses which may rarely produce psychotic schizophrenia-like symptoms, such as metabolic disturbance, systemic infection,syphilis, HIV infection, epilepsy, and brain lesions. Stroke, multiple sclerosis,hyperthyroidism, hypothyroidism anddementias such as Alzheimer's disease,Huntington's disease, frontotemporal dementia and Lewy Body dementia may also be associated with schizophrenia-like psychotic symptoms.[84] It may be necessary to rule out a delirium, which can be distinguished by visual hallucinations, acute onset and fluctuating level of consciousness, and indicates an underlying medical illness. Investigations are not generally repeated for relapse unless there is a specific medicalindication or possible adverse effects fromantipsychotic medication. In children hallucinations must be separated from normal childhood fantasies.[71]
Prevention
Prevention of schizophrenia is difficult as there are no reliable markers for the later development of the disease.[85] There is tentative evidence for the effectiveness of early interventions to prevent schizophrenia.[86] While there is some evidence that early intervention in those with a psychotic episode may improve short-term outcomes, there is little benefit from these measures after five years.[4] Attempting to prevent schizophrenia in the prodrome phase is of uncertain benefit and therefore as of 2009 is not recommended.[87] Cognitive behavioral therapy may reduce the risk of psychosis in those at high risk after a year[88]and is recommended by the National Institute for Health and Care Excellence (NICE) in this group.[89] Another preventative measure is to avoid drugs that have been associated with development of the disorder, includingcannabis, cocaine, and amphetamines.[1]

No comments:
Post a Comment